Let’s review Mr Mills’ details
Basic information
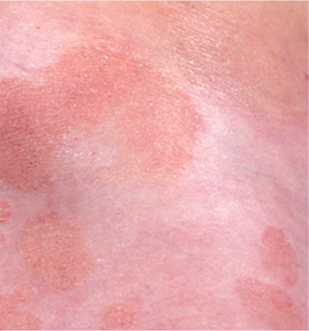
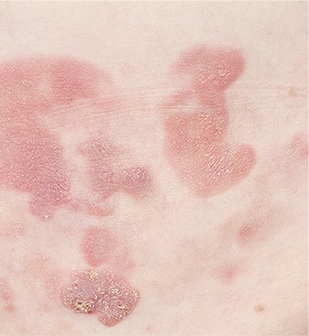
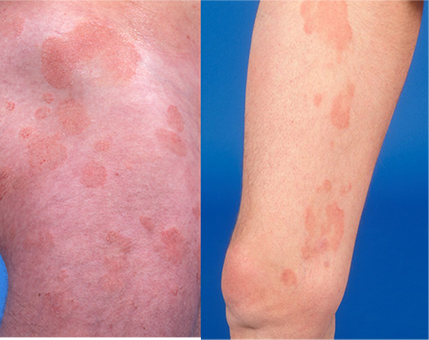
Presentation
Additional information from consultation
Unsatisfactory/incomplete response to corticosteroids6
Lesions on sun-protected sites1,2
Some level of improvement to lesions when exposed to sunlight9
Peripheral lymph node involvement1,2
Mr Mills‘ diagnosis
Mr Mills has a rare, serious and potentially life-threatening disease called mycosis fungoides (MF), a cutaneous T-cell lymphoma (CTCL) that can imitate many dermatological disorders.1-4,12
CTCLs are a heterogeneous group of extranodal non-Hodgkin’s lymphomas that are characterised by a cutaneous infiltration of malignant monoclonal T lymphocytes.1,13,14 MF accounts for around 60% of all CTCLs.15
Average time-to-diagnosis is around 4 years but can take decades in some instances.16 At early stage (patches and plaques), the disease is usually indolent, but 25% of patients progress to advanced stage in which the median life expectancy is only around 3 years.17,18
Sézary syndrome (SS) is another subtype of CTCL and it accounts for around 5% of cases.15,19 Patients with SS have erythroderma, lymphadenopathy, and blood involvement with clonally-related neoplastic T cells.15